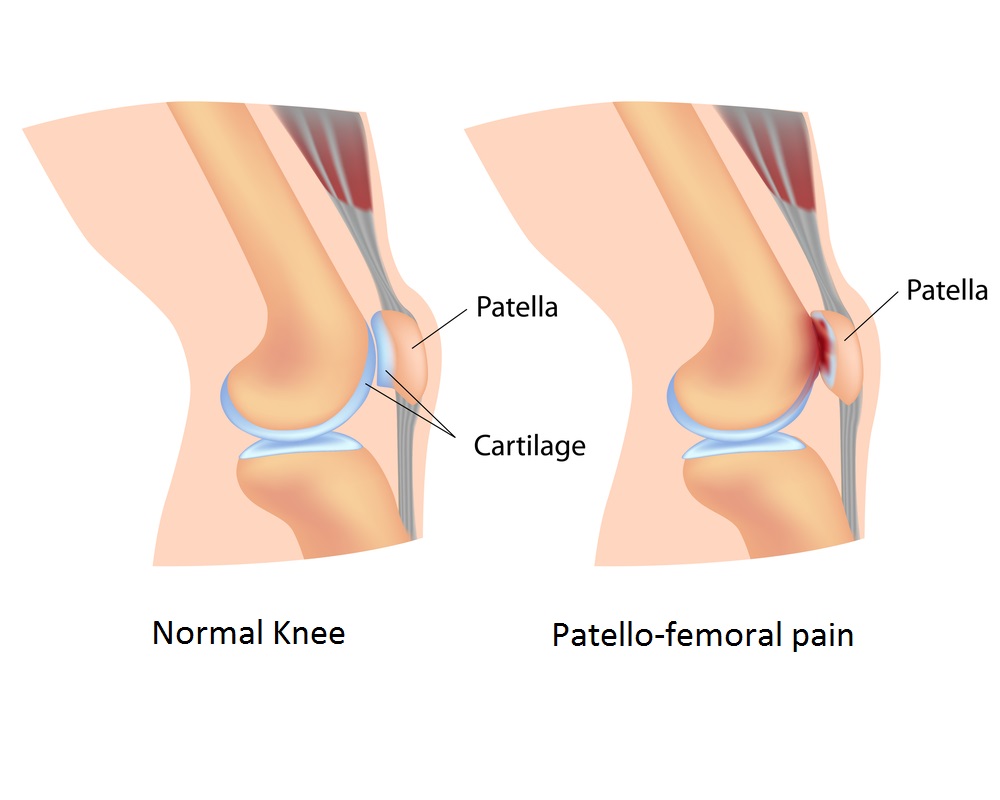
Patellofemoral Pain Syndrome: The last thing a runner *kneeds*
This is among the most common running-related injuries and involves dull achy pain in and around the kneecap


Runner’s knee may refer to a number of related conditions but most often, it’s associated with patellofemoral pain syndrome (PFPS). And as the number one cause of knee pain and the most common running-related injury, PFPS is a real pain for a lot of new and veteran runners alike.
RELATED: Demystifying runner’s knee
What is it?
PFPS is most commonly characterized by generalized (non-specific) pain behind or around the kneecap (patella), that most often occurs when climbing or descending stairs, squatting, kneeling, sitting with a flexed knee or during activities such as running or cycling. The irritation is often described as dull and achy but can also include short, sharp and shooting pain. Pain may present at all times but is often pronounced after prolonged periods of sitting and inactivity or during various physical activities. In some cases, it diminishes with activity only to return and intensify after cessation.
What causes it?
While the exact cause of PFPS can be difficult to determine, common causes include a change in training (Have you recently changed your volume or intensity?), frequently running up or down hills, adding strength training exercises or wearing worn-out shoes.
The injury is thought to result from increased pressure on the patellofemoral joint which may result from a combination of increased activity, malalignment of the patella during knee flexion, quadricep muscle imbalance and tight stabilizing structures such as the iliotibial band.
What should you do about it?
Treatment options vary, but the most sensible and immediately effective options include rest and elimination of activities that aggravate the knee joint. NSAIDS such as Advil may provide temporary relief but are not considered a long-term solution. Icing the knee and applying other anti-inflammation creams and gels may also provide some, and oftentimes temporary, relief. Taping and using a knee brace to stabilize the joint may be individually effective but are clinically insignificant.
Working to relax tight quadriceps, calves, shins, IT band and other muscles of the lower leg — through massage or foam rolling — as well as strengthening these muscles to correct imbalances may also prove pivotal to the successful long-term elimination of the condition.
In most cases, proper rest and rehab activities can eliminate a majority of pain within a matter of days or weeks, at which point, you can begin to gradually reintroduce training. In more rare cases, the pain can remain for months despite one’s best efforts to treat the condition and seeking further medical attention is warranted.